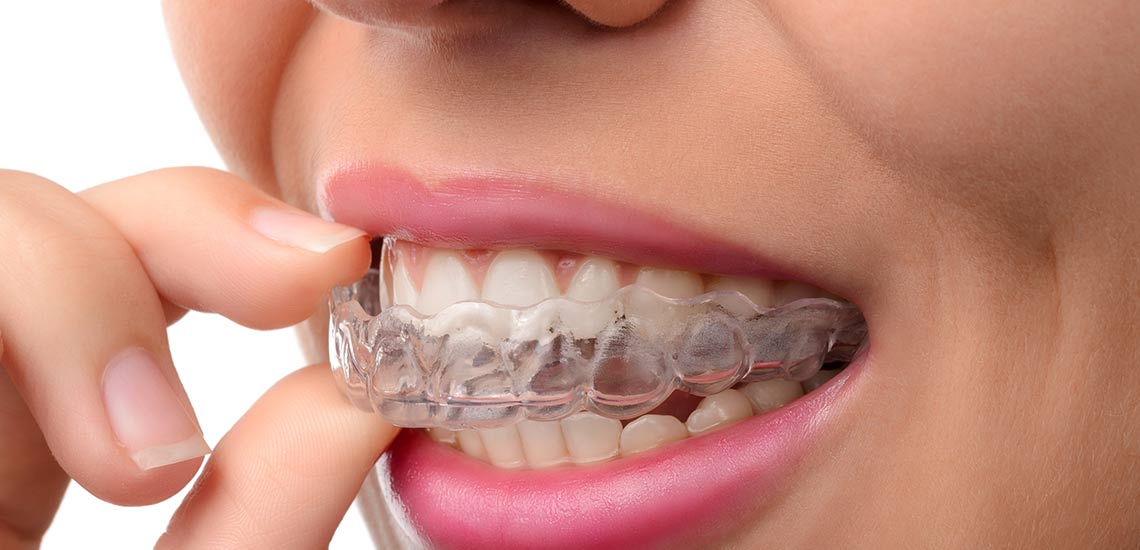
A mouthguard or nightguard is a protective device for the mouth that covers the teeth and gums to prevent and reduce injury to the teeth, arches, lips and gums. A mouthguard is most often used to prevent injury in contact sports, as a treatment for bruxism or TMD, or as part of certain dental procedures, such as tooth bleaching or sleep apnea. Depending on application, it may also be called a mouth protector, mouth piece, gumshield, gumguard, nightguard, occlusal splint, bite splint, or bite plane.
Occlusal splints (also called bite splints, bite planes, or night guards) are removable dental appliances carefully molded to fit the upper or lower arches of teeth.
They are used to protect tooth and restoration surfaces, manage mandibular (jaw) dysfunction TMD, and stabilize the jaw joints during occlusion or create space prior to restoration procedures. People prone to nocturnal bruxism, or nighttime clenching, as well as morsicatio buccarum may routinely wear occlusal splints at night. However, a meta-analysis of occlusal splints used for this purpose concluded "There is not enough evidence to state that the occlusal splint is effective for treating sleep bruxism. An indication of its use is questionable concerning sleep outcomes, but there may be some benefit with regard to tooth wear."
Occlusal splints are typically made of a heat-cured acrylic resin. Soft acrylic or light cured composite, or vinyl splints may be made more quickly and cheaply, but are not as durable, and are more commonly made for short-term use. Soft splints are also used for children because normal growth changes the fit of hard splints.
They cover all the teeth of the upper or lower arch, but partial coverage is sometimes used. Occlusal splints are usually used on either the upper or the lower teeth, termed maxillary splints or mandibular splints respectively, but sometimes both types are used at the same time. Maxillary splints are more common, although various situations favor mandibular splints.
Stabilizing or Michigan-type occlusal splints are generally flat against the opposing teeth, and help jaw muscle relaxation, while repositioning occlusal splints are used to reposition the jaw to improve occlusion.
Signs and symptoms
Most people who brux are unaware of the problem, either because there are no symptoms, or because the symptoms are not understood to be associated with a clenching and grinding problem. The symptoms of sleep bruxism are usually most intense immediately after waking, and then slowly abate, and the symptoms of a grinding habit which occurs mainly while awake tend to worsen through the day, and may not be present on waking. Bruxism may cause a variety of signs and symptoms, including:
- Excessive tooth wear, particularly attrition, which flattens the occlusal (biting) surface, but also possibly other types of tooth wear such as abfraction, where notches form around the neck of the teeth at the gumline.
- Tooth fractures, and repeated failure of dental restorations (fillings, crowns, etc.).
- Hypersensitive teeth, (e.g. dental pain when drinking a cold liquid) caused by wearing away of the thickness of insulating layers of dentin and enamel around the dental pulp.
- Inflammation of the periodontal ligament of teeth, which may make them sore to bite on, and possibly also a degree of loosening of the teeth.
- A grinding or tapping noise during sleep, sometimes detected by a partner or a parent. This noise can be surprisingly loud and unpleasant, and can wake a sleeping partner. Noises are rarely associated with awake bruxism.
- Other parafunctional activity which may occur together with bruxism: cheek biting (which may manifest as morsicatio buccarum and/or linea alba), and/or lip biting.
- A burning sensation on the tongue (see: glossodynia), possibly related to a coexistent "tongue thrusting" parafunctional activity.
- Indentations of the teeth in the tongue ("crenated tongue" or "scalloped tongue").
- Hypertrophy of the muscles of mastication (increase in the size of the muscles that move the jaw),[8] particularly the masseter muscle.
- Tenderness, pain or fatigue of the muscles of mastication, which may get worse during chewing or other jaw movement.
- Trismus (restricted mouth opening).
- Pain or tenderness of the temporomandibular joints, which may manifest as preauricular pain (in front of the ear), or pain referred to the ear (otalgia).
- Clicking of the temporomandibular joints.
- Headaches, particularly pain in the temples, caused by muscle pain associated with the temporalis muscle.
Bruxism is usually detected because of the effects of the process (most commonly tooth wear and pain), rather than the process itself. The large forces that can be generated during bruxism can have detrimental effects on the components of masticatory system, namely the teeth, the periodontium and the articulation of the mandible with the skull (the temporomandibular joints). The muscles of mastication that act to move the jaw can also be affected since they are being utilized over and above of normal function.
Tooth wear
Many publications list tooth wear as a consequence of bruxism, but some report a lack of a positive relationship between tooth wear and bruxism. Tooth wear caused by tooth-to-tooth contact is termed attrition. This is the most usual type of tooth wear that occurs in bruxism, and affects the occlusal surface (the biting surface) of the teeth. The exact location and pattern of attrition depends on how the bruxism occurs, e.g., when the canines and incisors of the opposing arches are moved against each other laterally, by the action of the medial pterygoid muscles, this can lead to the wearing down of the incisal edges of the teeth. To grind the front teeth, most people need to posture their mandible forwards, unless there is an existing edge to edge, class III incisal relationship. People with bruxism may also grind their posterior teeth (back teeth), which wears down the cusps of the occlusal surface. Once tooth wear progresses through the enamel layer, the exposed dentin layer is softer and more vulnerable to wear and tooth decay. If enough of the tooth is worn away or decayed, the tooth will effectively be weakened, and may fracture under the increased forces that occur in bruxism.
Abfraction is another type of tooth wear that is postulated to occur with bruxism, although some still argue whether this type of tooth wear is a reality.[9] Abfraction cavities are said to occur usually on the facial aspect of teeth, in the cervical region as V-shaped defects caused by flexing of the tooth under occlusal forces. It is argued that similar lesions can be caused by long-term forceful toothbrushing. However, the fact that the cavities are V-shaped does not suggest that the damage is caused by toothbush abrasion, and that some abfraction cavities occur below the level of the gumline, i.e., in an area shielded from toothbrush abrasion, supports the validity of this mechanism of tooth wear. In addition to attrition, erosion is said to synergistically contribute to tooth wear in some bruxists, according to some sources.
Tooth mobility
The view that occlusal trauma (as may occur during bruxism) is a causative factor in gingivitis and periodontitis is not widely accepted.It is thought that the periodontal ligament may respond to increased occlusal (biting) forces by resorbing some of the bone of the alveolar crest, which may result in increased tooth mobility, however these changes are reversible if the occlusal force is reduced. Tooth movement that occurs during occlusal loading is sometimes termed fremitus. It is generally accepted that increased occlusal forces are able to increase the rate of progression of pre-existing periodontal disease (gum disease), however the main stay treatment is plaque control rather than elaborate occlusal adjustments. It is also generally accepted that periodontal disease is a far more common cause of tooth mobility and pathological tooth migration than any influence of bruxism, although bruxism may much less commonly be involved in both.
Pain
Most people with bruxism will experience no pain. The presence or degree of pain does not necessarily correlate with the severity of grinding or clenching. The pain in the muscles of mastication caused by bruxism can be likened to muscle pain after exercise. The pain may be felt over the angle of the jaw (masseter) or in the temple (temporalis), and may be described as a headache or an aching jaw. Most (but not all) bruxism includes clenching force provided by masseter and temporalis muscle groups; but some bruxers clench and grind front teeth only, which involves minimal action of the masseter and temporalis muscles. The temporomandibular joints themselves may also become painful, which is usually felt just in front of the ear, or inside the ear itself. Clicking of the jaw joint may also develop. The forces exerted on the teeth are more than the periodontal ligament is biologically designed to handle, and so inflammation may result. A tooth may become sore to bite on, and further, tooth wear may reduce the insulating width of enamel and dentin that protects the pulp of the tooth and result in hypersensitivity, e.g. to cold stimuli.
The relationship of bruxism with temporomandibular joint dysfunction (TMD, or temporomandibular pain dysfunction syndrome) is debated. Many suggest that sleep bruxism can be a causative or contributory factor to pain symptoms in TMD. Indeed, the symptoms of TMD overlap with those of bruxism. Others suggest that there is no strong association between TMD and bruxism. A systematic review investigating the possible relationship concluded that when self-reported bruxism is used to diagnose bruxism, there is a positive association with TMD pain, and when stricter diagnostic criteria for bruxism are used, the association with TMD symptoms is much lower. In severe, chronic cases, bruxism can lead to myofascial pain and arthritis of the temporomandibular joints.